2 results
Impact of measurement and feedback on chlorhexidine gluconate bathing among intensive care unit patients: A multicenter study
- Yoona Rhee, Mary K. Hayden, Michael Schoeny, Arthur W. Baker, Meghan A. Baker, Shruti Gohil, Chanu Rhee, Naasha J. Talati, David K. Warren, Sharon Welbel, Karen Lolans, Bardia Bahadori, Pamela B. Bell, Heilen Bravo, Thelma Dangana, Christine Fukuda, Tracey Habrock Bach, Alicia Nelson, Andrew T. Simms, Pam Tolomeo, Robert Wolf, Rachel Yelin, Michael Y. Lin, for the CDC Prevention Epicenters Program
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 9 / September 2023
- Published online by Cambridge University Press:
- 13 September 2023, pp. 1375-1380
- Print publication:
- September 2023
-
- Article
- Export citation
-
Objective:
To assess whether measurement and feedback of chlorhexidine gluconate (CHG) skin concentrations can improve CHG bathing practice across multiple intensive care units (ICUs).
Design:A before-and-after quality improvement study measuring patient CHG skin concentrations during 6 point-prevalence surveys (3 surveys each during baseline and intervention periods).
Setting:The study was conducted across 7 geographically diverse ICUs with routine CHG bathing.
Participants:Adult patients in the medical ICU.
Methods:CHG skin concentrations were measured at the neck, axilla, and inguinal region using a semiquantitative colorimetric assay. Aggregate unit-level CHG skin concentration measurements from the baseline period and each intervention period survey were reported back to ICU leadership, which then used routine education and quality improvement activities to improve CHG bathing practice. We used multilevel linear models to assess the impact of intervention on CHG skin concentrations.
Results:We enrolled 681 (93%) of 736 eligible patients; 92% received a CHG bath prior to survey. At baseline, CHG skin concentrations were lowest on the neck, compared to axillary or inguinal regions (P < .001). CHG was not detected on 33% of necks, 19% of axillae, and 18% of inguinal regions (P < .001 for differences in body sites). During the intervention period, ICUs that used CHG-impregnated cloths had a 3-fold increase in patient CHG skin concentrations as compared to baseline (P < .001).
Conclusions:Routine CHG bathing performance in the ICU varied across multiple hospitals. Measurement and feedback of CHG skin concentrations can be an important tool to improve CHG bathing practice.
Admission and Discharge Sampling Underestimates Multidrug-Resistant Organism (MDRO) Acquisition in an Intensive Care Unit
- Sarah Sansom, Michael Lin, Christine Fukuda, Teppei Shimasaki, Thelma Dangana, Nicholas Moore, Rachel Yelin, Yoona Rhee, Lina Tabith, Jianrong Sheng, Enrique Cornejo Cisneros, John Murray, Kyle Chang, Karen Lolans, Michelle Ariston, William Rotunno, Hazel Ramos, Haiying Li, Khaled Aboushaala, Naomi Iwai, Christine Bassis, Vincent Young, Mary Hayden
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s28
-
- Article
-
- You have access Access
- Open access
- Export citation
-
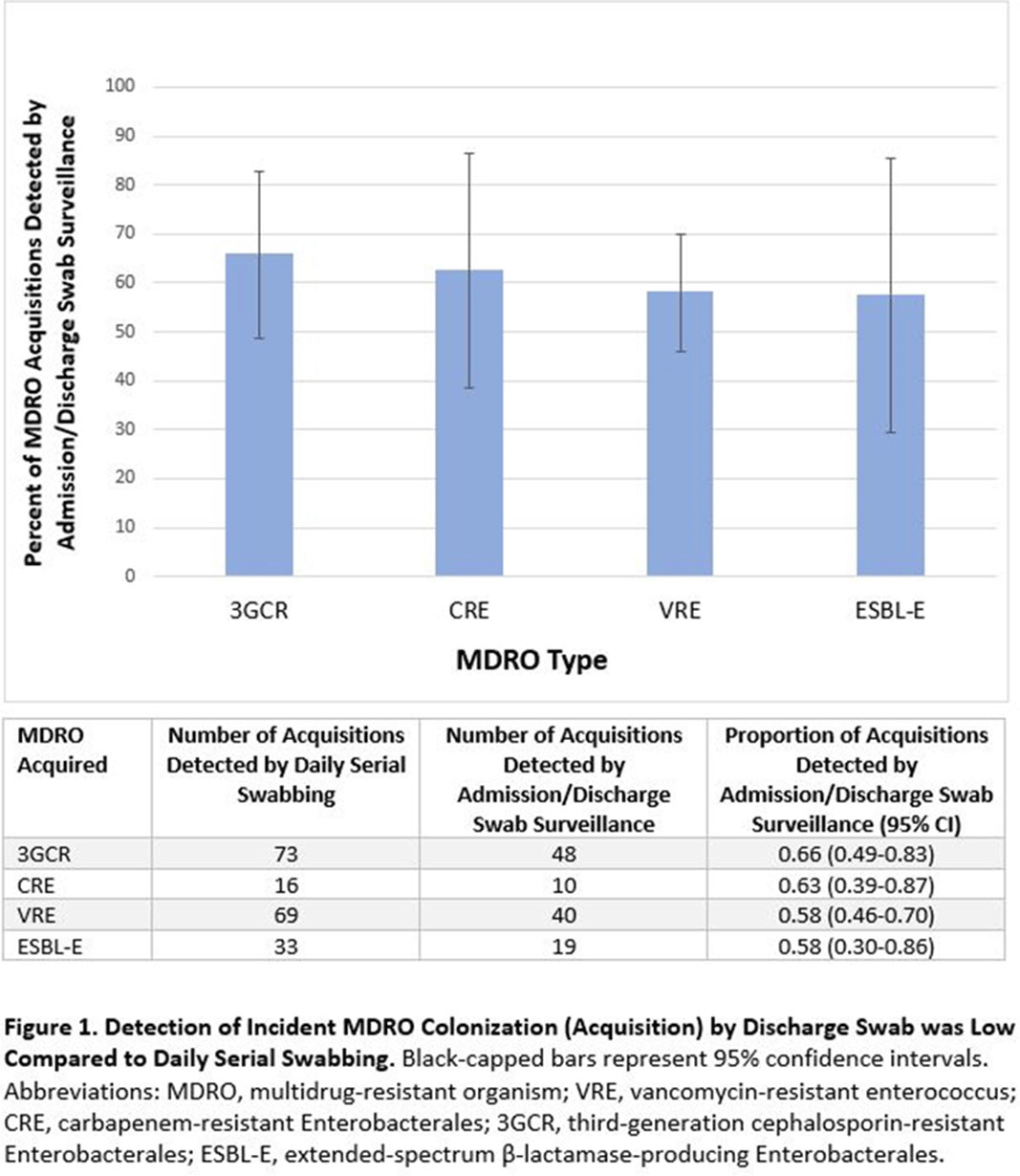
Background: Identification of hospitalized patients with enteric multidrug-resistant organism (MDRO) carriage, combined with implementation of targeted infection control interventions, may help reduce MDRO transmission. However, the optimal surveillance approach has not been defined. We sought to determine whether daily serial rectal surveillance for MDROs detects more incident cases (acquisition) of MDRO colonization in medical intensive care unit (MICU) patients than admission and discharge surveillance alone. Methods: Prospective longitudinal observational single-center study from January 11, 2017, to January 11, 2018. Inclusion criteria were ≥3 consecutive MICU days and ≥2 rectal or stool swabs per MICU admission. Daily rectal or stool swabs were collected from patients and cultured for MDROs, including vancomycin-resistant Enterococcus (VRE), carbapenem-resistant Enterobacterales (CRE), third-generation cephalosporin-resistant Enterobacterales (3GCR), and extended-spectrum β-lactamase–producing Enterobacterales (ESBL-E) (as a subset of 3GCR). MDRO detection at any time during the MICU stay was used to calculate prevalent colonization. Incident colonization (acquisition) was defined as new detection of an MDRO after at least 1 prior negative swab. We then determined the proportion of prevalent and incident cases detected by daily testing that were also detected when only first swabs (admission) and last swabs (discharge) were tested. Data were analyzed using SAS version 9.4 software. Results: In total, 939 MICU stays of 842 patients were analyzed. Patient characteristics were median age 64 years (interquartile range [IQR], 51–74), median MICU length of stay 5 days (IQR, 3–8), median number of samples per admission 3 (IQR, 2–5), and median Charlson index 4 (IQR, 2–7). Prevalent colonization with any MDRO was detected by daily swabbing in 401 stays (42.7%). Compared to daily serial swabbing, an admission- and discharge-only approach detected ≥86% of MDRO cases (ie, overall prevalent MDRO colonization). Detection of incident MDRO colonization by an admission- or discharge-only approach would have detected fewer cases than daily swabbing (Figure 1); ≥34% of total MDRO acquisitions would have been missed. Conclusions: Testing patients upon admission and discharge to an MICU may fail to detect MDRO acquisition in more than one-third of patients, thereby reducing the effectiveness of MDRO control programs that are targeted against known MDRO carriers. The poor performance of a single discharge swab may be due to intermittent or low-level MDRO shedding, inadequate sampling, or transient MDRO colonization. Additional research is needed to determine the optimal surveillance approach of enteric MDRO carriage.
Funding: No
Disclosures: None
Figure 1.